The US Centers for Disease Control and Prevention released this week its updated guidance for operating youth and summer camps during COVID-19. Tucked between sections on vaccination, mask use, and new distancing guidelines is a small piece on “Health equity considerations in prevention strategies.”
The presence of this sidebar, which notes “The COVID-19 pandemic has brought social and racial injustice and inequity to the forefront of public health,” would have been unimaginable in a previous US administration. Even though the piece is brief, and graphically set off from the bulk of the public health guidance updates for camps, its presence is an important recognition that safety and health issues disproportionately affect those who are members of groups that have been systemically oppressed and disenfranchised.
These groups include those not of the dominant race, religion, citizenship status, ethnicity, national origin, or gender identity, among other characteristics.
The disproportionate effect COVID-19 has on racial and ethnic minorities, in particular, has been previously documented.
The CDC has previously noted that health equity– when all members of society enjoy a fair and just opportunity to be as healthy as possible—is still not a reality, as COVID-19 has unequally affected many racial and ethnic minority groups, due to factors such as racism and other forms of discrimination systemically embedded in health care, housing, education, criminal justice, and finance.
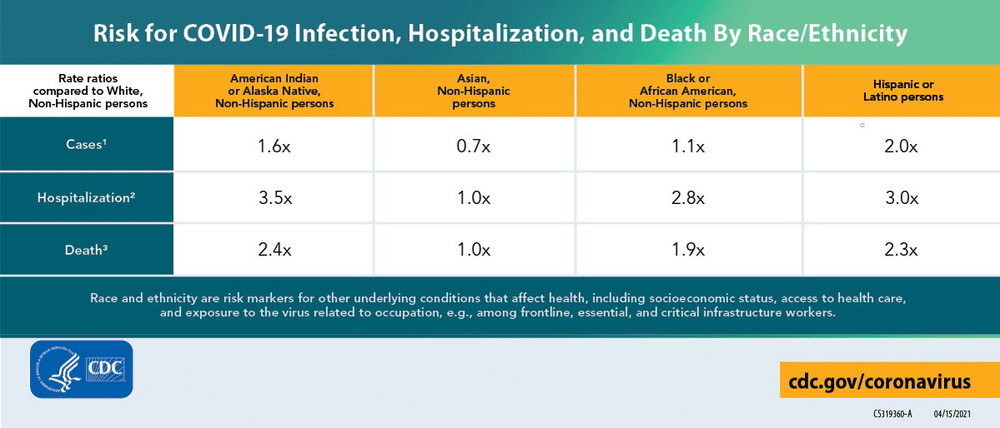
The corrosive stress of dealing with racism can have a negative impact on the body, increasing the risk of severe illness with COVID-19. Structural barriers to access to health insurance, medical care, high-quality medical care, education, housing, healthy food, and protection from pollution exposure lead to African Americans, Hispanics/Latinos, Native Americans, and Alaskan Natives becoming sick and dying from COVID-19 at rates higher than whites or the general population. For example, Blacks, Latinos, and American Indians have experienced hospitalization at more than double or triple the rate of non-Hispanic whites.
Health inequity results from poverty, structural racism, discrimination and disinvestment in many communities of color—including, in the outdoor context, reduced access to parks for healthful outdoor recreation.
This is not new. However, what does seem new is the embedding of health equity issues in general public health guidance—in this case, COVID-19 safety for camps and related outdoor programs.
Health Equity for Outdoor Programs
What can we do to promote health equity?
The CDC encourages outdoor program managers to promote health equity to ensure participants have resources to maintain and manage their physical and mental health. Camp and other outdoor programs are encouraged to:
- Design programs to meet the physical, spiritual and mental health needs of participants
- Support faith, family and cultural bonds (for example, through inclusive program design)
- Foster support and connection, even when physically apart
- Provide information on COVID-19 prevention and mitigation
- Support easy access to information, affordable testing, and medical care, as possible
- Provide healthy food
- Provide written materials in multiple languages
- Support staff with health equity best practices such as flexible leave policies, health and safety training, implicit bias training, PPE access, and capacity to engage in physical distancing and other good public health measures
The CDC also encourages outdoor program managers to adapt prevention strategies when caring for people with disabilities, such as:
- Being aware of challenges with mask-wearing for people with sensory, cognitive, or behavioral issues
- Disinfecting wheelchairs and other assistive devices
- Understanding that people with disabilities may be at increased risk of severe illness from COVID-19, and may have difficulty accessing and understanding safety information or practicing preventive measures like hand-washing
Although much more work urgently needs to be done to address equity—including health equity—in outdoor programs, the CDC’s embedding of health equity guidance in COVID-19 prevention and mitigation resources is an important and positive step in the right direction.
Going Beyond Health Equity
In addition to promoting health equity and support for people with disabilities, outdoor programs can take steps such as:
- Reducing financial, logistical, cultural and other barriers to access for outdoor programs
- Recruiting, hiring, training and supporting a staff team representative of diverse participant populations
- Providing robust, evidence-based staff training on equity and inclusion
- Building equity and inclusion into outdoor program curriculum
- Building inclusion into program administration, such as marketing strategies, promotional materials, sleeping accommodations, space for religious observance, toilet and changing facilities, and food service, among others
Doing these things well can be enormously difficult—psychologically, intellectually, financially and otherwise—but are nonetheless vital. Difficulties stem from humans’ natural tendency towards tribalism and “othering” those who do not look or act like them, and systemic inequities throughout society, on which individual outdoor programs have limited influence, but which those programs cannot easily escape.
Yet, each of us has a responsibility to do what we can, within our capacities, to support equity and inclusion in our outdoor programs.
COVID-19 Guidance for Camps
The CDC update released this week does more than recognize health equity issues in camp and other outdoor programs. The updated guidance covers good general public health practices, including:
- Getting vaccinated when eligible
- Staying home if sick
- Using masks
- Physical distancing, including cohorting
- Handwashing
- Engaging in outdoor activities whenever possible
- Increasing ventilation for indoor activities
- Cleaning and disinfecting
- Contact tracing, isolation and quarantine
The update emphasizes the use of these prevention strategies to control the spread of new COVID-19 variants. Much of the guidance remains the similar to what the CDC published in the earlier days of the pandemic, with the exception of removing information on physical barriers, and emphasizing vaccination, which was not an option in the USA until December 2020.
The new guidance emphasizes that all people in camp facilities should wear masks at all times with exceptions for certain people (such as children under 2 or those whose disability prevents safe mask use), or for certain settings or activities, such as while eating and drinking or swimming.
(Uneven mask-wearing in camps has been documented as a problem, perhaps most notoriously at a camp that engaged in maskless indoor singing and cheering, resulting in the closure of the camp four days after it opened, with 76 percent of attendees testing positive for the virus causing COVID-19.)
The guidance reinforces the standard of six-foot physical distancing, but introduces a three-foot guideline between campers within a cohort.
A PDF copy of the 14-page CDC update is available here.
Support from Viristar
Viristar offers a free mini-course on how outdoor programs can manage risks of COVID-19, covering general principles, best medical practices, and systems-informed responses to the pandemic.
Viristar also provides an industry-leading Risk Management for Outdoor Programs 40-hour online training course. This covers the same COVID-19 topics but also provides a comprehensive training on best practices for experiential, wilderness, adventure, travel-based and outdoor programs to assess and mitigate risk in their programs. The course offers a systems-based approach and covers human factors in incident causation, emergency response, risk management plans, and much more. More information and a course schedule are available here.



